Research in global health emergencies: ethical issues
Report
Published 28/01/2020

Developing an ethical compass
See Chapter 4 of the full report
Research in global health emergencies presents difficult ethical challenges for a number of reasons – for example:
- because decisions made at policy level can make it difficult to act ethically on the ground;
- because of uncertainty about how and whether ‘standard’ ethical frameworks still apply in these uniquely challenging circumstances; and
- because practitioners from different disciplines are guided by different (and at times competing) ethical frameworks.
Questions raised by conflicting obligations and deadlines
- How should studies of new treatments balance the interests of individuals (who may want the chance to access experimental forms of care straight away) and the wider interests of communities (who may benefit more in the long term from rapid and decisive research results about effectiveness)?
- Should individuals be given a choice of opting out of research that is concerned with public good, such as using routine patient data to improve health systems?
- How do research organisations negotiate the interests of their workers, and those of research participants, for example, in health and safety requirements in inherently dangerous situations?
- How do researchers manage conflicting lines of accountability – e.g., to the communities they are working with, national governments, their funders and employers, and their own professional standards?
There is no simple answer to any of these questions. We propose an ‘ethical compass’ of three widely shared values, to help guide policy approaches, and provide a common language for thinking through ethical dilemmas arising on the ground. The ethical compass was developed in the light of the experiences and evidence shared by those who contributed to our inquiry.
Using the compass
In many cases the three values of equal respect, fairness, and helping reduce suffering will point in the same direction, leading to a clear course of action. Where this is not the case, a decision about whether to proceed with research will need a careful, inclusive, and transparent decision-making process, and independent review. The question ‘What best helps reduce suffering?’ will always be important. However, considerations of what is fair, and what shows equal respect, must also influence the way research is conducted.
The three values provide a tool for thinking through whether it is acceptable to adapt standard ethical principles in any way. Possible approaches include:
- Interpreting principles in the light of the features of the emergency – for example aiming to develop community engagement processes as the research develops, when the situation is too urgent to build up processes before the start;
- Recognising additional principles from partners’ ethical traditions or in response to local needs – for example including a tier of community consent to research, as well as individual consent, and taking account of local traditions; and
- Taking action to strengthen other parts of the ethics ‘ecosystem’ in cases where standard principles alone cannot provide the degree of protection required – for example, thinking about how participants’ interests can be protected in circumstances where people might feel they have no choice but to consent to research participation.
These decisions will need to be taken on a case-by-case basis depending on the features of each emergency, but should always be guided by consideration of the three values.
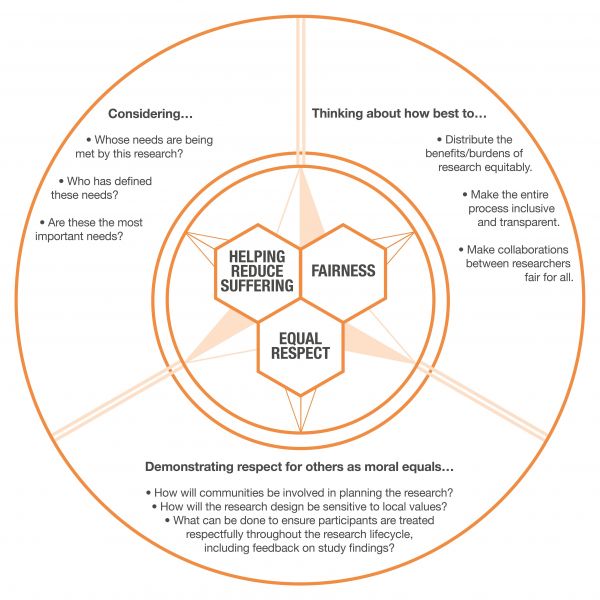
An ethical compass to guide decision-making
Who has a duty to take action?
People and organisations may have an ethical duty to take action:
- if they have the greatest ability to act;
- if their relationship with others (for example as an employer) gives them special responsibilities; or
- if their actions or failings mean that they have a degree of culpability for the effects of the emergency (for example through negligent failure to prevent it or mitigate the effects).
‘Duty-bearers’ include governments, intergovernmental organisations, humanitarian organisations, research funders, employers of researchers, and journals. The three values of fairness, equal respect, and helping reduce suffering should underpin the approach that these duty-bearers take at policy level, so that they are able to support ethical research during emergencies. Many of these duty-bearers also have duties to plan for the future, to minimise or prevent the impact of future emergencies through strengthening health and health research systems.

Share